How Ketamine Works to Treat Depression
Standard antidepressants (such as Prozac, and others) work on a group of chemical messengers and pathways in the brain called the serotonin system. Researchers once thought that a lack of serotonin was the cause of depressive illness, and that these medications worked by simply boosting serotonin levels in the brain.
More recent research suggests a more complicated explanation: serotonin medications work in part by stimulating the production of growth factors and new proteins inside brain cells, which eventually help form new connections within the pathways of the brain. But creating new brain cell growth factors and proteins takes time — a few weeks, at least — which is thought to explain the typical expected delay in response to antidepressant medications, for the most part.
Ketamine treatment works on a different neurochemical system in the brain – the glutamate system. Researcher Ron Duman at Yale University believes ketamine rapidly increases the communication among existing brain cells by creating new connections among them. This is a quicker process than waiting for new neurons to form growth factors within the serotonin pathway, and accomplishes the same goal of enhancing brain circuit activity.
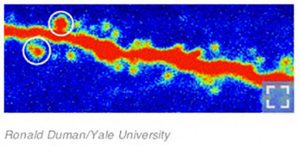
To study how this might work, Dr. Duman looked at Ketamine’s effect on rat brains. The first image below shows the brain cell of a rat (in red) that has received no ketamine treatment. The small bumps and spots on the side of the neuron (circled) are budding connections between brain cells.
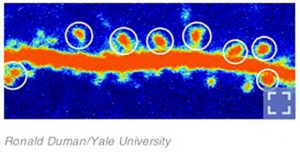
Within hours of giving the rats doses of ketamine, Dr. Duman saw a dramatic increase in the number of new connections sprout up between brain cells. It is this increase in brain cell connectivity that is thought to bring on Ketamine’s antidepressant response.
Why Ketamine vs. ECT or TMS?
ECT, Electroconvulsive Therapy, has for decades been a dramatic treatment for severe psychiatric disorders, principally for depression that is unresponsive to psychotherapy and antidepressant medications (known as Treatment Resistant Depression). ECT typically involves a hospitalized patient periodically receiving brief electrical pulses over the scalp while completely under anesthesia, usually every other day for a week or two. If improved, a patient can be transitioned to outpatient hospital-based ECT sessions every other day for a week or so. Patients are then put on antidepressant medication, and followed as a regular patient would be from then on for outpatient medication management. However, most people will eventually relapse into depression at some point, necessitating re-hospitalization and more rounds of ECT treatment as before over the course of several weeks. Obviously, a patient undergoing ECT will be off work for several weeks, staying in the hospital for some time, will be under anesthesia several times a week, and will incur bills for hospitalization, psychiatrist fees, and anesthesiologist fees (these are covered by medical insurance, minus your deductible). Notable potential side effects of ECT treatment include persistent memory loss. However, ECT is the current gold-standard for severe depression, and remarkably effective for the vast majority of patients.
TMS (Transcutaneous Magnetic Stimulation) is a fairly new treatment for mild to moderate depression, whose clinical effectiveness remains unclear. The FDA, controversially, approved the use of a TMS device in 2011. This device consists of a handheld magnetic coil that is placed on the scalp to induce small amounts of electrical activity while in an outpatient office setting. No anesthesia or specific safety precautions seem necessary, and a patient typically undergoes a one hour treatment session daily, 5 days per week, for 4 to 6 weeks (approximately 20 to 30 treatment sessions total). Very few insurance companies pay for TMS because of its controversial effectiveness, and an entire treatment course can therefore cost $10,000 to $20,000 out of pocket over the course of the 4 to 6 weeks of treatment. Most studies suggest that TMS therapy takes several weeks to work (just like typical antidepressant medications), and is ultimately no more effective than simply switching your antidepressant medication. Ultimately, it is not known at this point whether TMS can be used to treat depression for the long term, or if a patient may require periodic re-treatment in the future.
Ketamine, in contrast to ECT and TMS, has a very rapid and robust antidepressant (and anti-suicidal) effect. Like ECT, the data supporting ketamine therapy for Treatment Resistant Depression, are solid and unequivocal, and have proven value in very hard-to-treat depression. TMS, in contrast, does not have strong data to support its effectiveness, even in non-severe depression, and takes several weeks to work. Both ECT and TMS can be quite expensive (costs of hospitalization, days off work, etc.) compared to Ketamine. Like TMS, Ketamine therapy can be done in an outpatient office setting without anesthesia and with minimal hassle and side effects.
However, the one thing that Ketamine, ECT, and TMS have in common is that they likely all will require continued use of antidepressant medications for relapse prevention over time.
We here at Southlake Psychiatric and Counseling Center in Southlake, Texas use a modified treatment protocol based off of the existing data reported in the clinical trials in the medical literature to help those with Treatment Resistant Depression get better in the quickest time possible. In comparison to the many “Ketamine Clinics” that are cropping up in the last couple of years that are run by Anesthesiologists, Dr. William T. Goldman is a Board-Certified Psychiatrist, well-versed in the diagnosis and treatment of psychiatric conditions in general, and in Treatment Resistant Depression specifically. Dr. Goldman has been utilizing Ketamine for his patients for over 6 years now, performing hundreds of treatments. Anesthesiologists are not qualified to diagnose or treat psychiatric patients, as psychiatrists are not qualified to anesthetize patients undergoing surgery.